Buruli ulcer is a chronic, debilitating infection caused by the bacterium Mycobacterium ulcerans. It belongs to the same family of bacteria as tuberculosis and leprosy, highlighting its significance as a public health concern. The bacteria produce a unique toxin called mycolactone, which not only destroys tissue but also suppresses the immune system, effectively allowing the infection to progress unnoticed. This insidious nature means that the infection is often painless in its early stages, leading individuals to delay seeking medical attention until more severe symptoms manifest, such as painful ulcers and skin lesions. Understanding the mechanisms of Mycobacterium ulcerans and increasing awareness about Buruli ulcer are crucial for timely diagnosis and treatment, ultimately improving patient outcomes and reducing the burden of this neglected tropical disease.
Causes & Transmission
The exact mode of transmission is still a subject of intense research. Unlike many other diseases, it is not spread from person to person, which distinguishes it from many infectious ailments that require human-to-human contact for propagation. This characteristic has led scientists to explore other potential vectors and environmental triggers for infection.
Environmental Sources
Buruli ulcer, caused by the bacterium Mycobacterium ulcerans, primarily thrives in specific environmental conditions. The bacteria are found in slow-moving or stagnant water, such as swamps, ponds, and wetlands. These habitats provide a suitable environment for the bacteria to flourish, especially in warmer climates. Individuals who frequently engage in activities near or in these types of water bodies, such as fishing, swimming, or agricultural work, may be at a heightened risk of exposure.
Insect Links
Moreover, researchers have identified potential insect links to the transmission of Buruli ulcer, particularly in regions like Australia. Studies have shown a strong correlation between mosquitoes and Buruli ulcer, suggesting that these insects may play a significant role as carriers of the bacteria. The exact mechanism by which they transfer the bacteria to humans remains under investigation, yet this connection raises important public health considerations, highlighting the need for vector control in affected areas.
Skin Trauma
Another crucial aspect of the infection process involves skin trauma. It is believed that the bacteria enter the body through minor cuts or abrasions after contact with contaminated water or soil. Even seemingly insignificant injuries can serve as entry points for the bacteria, which is why people in endemic regions are advised to take precautionary measures, such as wearing protective clothing and promptly cleaning any wounds. Understanding how the bacteria penetrate the skin helps inform prevention strategies and encourages further studies on the risk factors associated with this debilitating disease.
Research continues to unravel the complexities of Buruli ulcer transmission, fostering a deeper understanding of its environmental and biological factors, ultimately contributing to more effective preventive measures and treatments.
Signs and Symptoms
The disease usually starts as a painless swelling. Because it doesn’t hurt, many people delay seeking treatment.
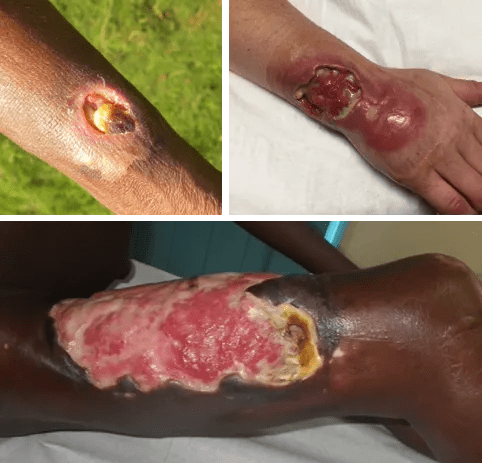
Stage 1 (Nodule/Plaque): A small, painless bump under the skin, often on the arms or legs.
Stage 2 (Ulceration): The bump breaks open into a large, “undermined” ulcer—meaning the hole under the skin is much larger than the opening on the surface.
Stage 3 (Complications): If untreated, the infection can reach the bone, leading to severe scarring, contractures (permanent shortening of muscles), or even the need for amputation.
Treatment Options
The treatment for Buruli ulcer has improved significantly over the last decade, moving away from surgery toward medication.
Antibiotics: A combination of Rifampicin and Streptomycin (or Clarithromycin) for 8 weeks is the standard treatment recommended by the World Health Organization (WHO).
Wound Care: Specialized dressings and cleaning are required to help the large ulcers heal and prevent secondary infections.
Surgery: Only used in severe cases to remove dead tissue, skin grafts, or to correct deformities.
Physiotherapy: Essential to prevent joints from locking up as the skin scars and tightens.
Prevention and Health Advice
Because the exact transmission of the virus is unknown, there is no specific vaccine or “sure-fire” prevention method available at this time. However, health officials unanimously recommend the following precautionary measures to reduce the risk of exposure:
Protect Your Skin
When working in endemic areas, especially near swamps or during farm activities, it is crucial to protect your skin. Wearing long-sleeved shirts and trousers not only provides a physical barrier against potential bites from insects but also reduces the risk of direct contact with any contaminated surfaces. Opt for light-colored clothing, as darker shades can attract more insects. Consider treating your clothing with permethrin, an insect repellent designed for fabric, to further enhance your protection.
Clean Wounds Immediately
It is essential to promptly attend to any injuries, no matter how minor they may seem. Immediately wash all cuts, scrapes, and wounds with soap and clean water to remove any dirt or pathogens. After thoroughly cleaning the area, cover the wound with a sterile bandage to protect it from potential infection. Regularly check the status of your wounds and change dressings as needed to maintain cleanliness and avoid complications.
Use Insect Repellent
Given that mosquitoes are suspected carriers of the virus in some regions, employing insect repellent is a vital step in prevention. Use repellents that contain DEET, as studies have shown they are effective in keeping these pests at bay. Apply the repellent on exposed skin and follow the instructions for reapplication, especially if you’ll be outside for an extended period. Additionally, consider using screens on windows and doors, and sleep under insecticide-treated bed nets if you are in a high-risk area.
By following these recommended practices, individuals can significantly reduce their risk of exposure to the virus until more specific preventive measures are developed. Staying informed and vigilant is key to personal safety in areas where such health threats are present.
Leave a comment